Supraventricular Arrhythmias
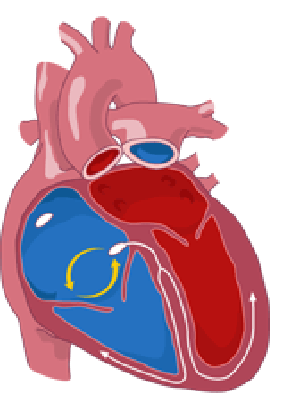
Supraventricular arrhythmias are tachycardias (fast heart rates) that start in the atria or the atrioventricular node (cells located between the atria and the ventricles) and occur from time to time (paroxysmal). Types of supraventricular arrhythmias include atrial fibrillation (AF), atrial flutter, paroxysmal supraventricular tachycardia (PSVT), and Wolff-Parkinson-White (WPW) syndrome.
Causes
Normally, the chambers of the heart (atria and ventricles) contract in a coordinated manner. The contractions are caused by an electrical signal that begins in the sinoatrial node (also called the sinus atrial (SA) node).
The signal is conducted through the atria (the upper heart chambers) and stimulates the atria to contract. Paroxysmal supraventricular tachycardia (PSVT) can be initiated in the SA node; in the atria or the atrial conduction pathways; or in the AV node. It may occur at any age but is mostly seen in young people and infants. PSVT can occur with digitalis toxicity. It can be a form of a re-entry tachycardia (an electrical current is caught in a reentrant loop, excessively stimulating the heart), as in the case of Wolff-Parkinson-White syndrome.
Symptoms of Supraventricular Arrhythmia
These symptons are a sign of supraventricular arrhythmia. It should be noted that symptoms may start and stop suddenly, and can last for a few minutes or several hours. A PSVT lasting more than 50% of the day is considered an incessant PSVT.
• Anxiety, feeling of impending doom
• Shortness of breath
• Chest Tightness
Additional symptoms that may be associated with this disease include fainting and dizziness.
Exams and Tests
An examination during a PSVT episode detects a rapid heart rate. The heart rate may be 150 to 250 beats per minute (bpm) (in children the heart rate tends to be very high). There may be signs of poor perfusion (blood circulation) such as light-headedness. Between episodes of PSVT, the heart rate is normal (60 to 100 bpm).
Additional info
• An ECG during symptoms shows PSVT.
• Because of the sporadic nature of the PSVT, its diagnosis may require continuous ambulatory monitoring. The most common is the 24-hour Holter monitoring. For longer recording periods, a "loop recorder" (with computer memory) is used.
• An electrophysiology study (EPS) is often necessary for an accurate diagnosis, and to recommend the best treatment.
Treatment
PSVT can occur with few or no symptoms, and may not require treatment. If symptoms occur or there are underlying cardiac disorders, treatment may be necessary. People having an episode of PSVT can try to interrupt the episode with a Valsalva maneuver.
This consists of holding the breath and straining (pushing with the abdomen as if to provoke a bowel movement) or coughing while sitting with the upper body bent forward. Splashing ice water on the face has been reported by some people as helpful. Persons having an episode of PSVT may be offered therapy to interrupt the arrhythmia and convert it to a normal sinus rhythm. In the emergency room, a health care provider may massage the carotid arteries in the neck in an attempt to interrupt the arrhythmia. Caution -- do not try this at home! This technique can cause severe slowing of the heart rate. Electrical cardioversion (shock) is successful in conversion of PSVT to a normal sinus rhythm in many cases. Another way to rapidly convert a PSVT is to administer intravenous medications, including adenosine and verapamil. Other medications may be used, such as procainamide, beta-blockers, and propafenone.
Aside from treating isolated episodes of PSVT, some patients may require a long-term or definitive treatment of the PVST which is directed toward the prevention or complete eradication of further episodes or arrhythmia. Such long-term treatment includes:
Long-term Treatment
• Daily medications -- such as B blockers, calcium channel blockers, digoxin or antiarrhythmics.
• Radiofrequency catheter ablation -- currently the treatment of choice for most PSVT's.
• Surgical modification of the electrical conduction pathway (the pathways in the heart that conduct the impulse to contract) -- this may be recommended in some cases when other heart surgery for other reasons is also indicated.
• Pacemakers -- very occasionally used in children with PSVT who have not responded to any other treatment. The pacemaker is designed to interrupt (override) the tachycardia.
Acknowledgements
Heart Rhythm Specialists of South Florida gives special thanks to the National Library of Medicine and National Heart Lung and Blood Institute whose Web sites aided in the research of the patient educational material provided above.