Electrophysiology Study
Intracardiac electrophysiology study (EPS) involves placing wire electrodes within the heart to determine the characteristics of heart arrhythmias.
How test is performed
The study is performed in a hospital laboratory by a trained staff that includes cardiologists, technicians, and nurses. The environment is safe and controlled to minimize any danger or risk to the patient.
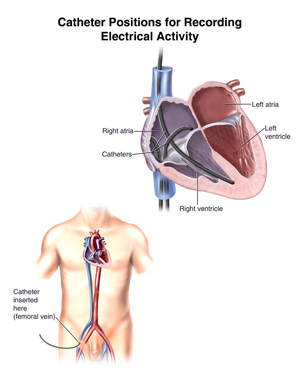
The cardiologist inserts a catheter into a vein through a small incision in the groin after cleansing the area and numbing it with a local anesthetic. This catheter is equipped with an electrode connected to electrocardiographic monitors.
The catheter is then carefully threaded into the heart using an x-ray imaging technique called fluoroscopy to guide the insertion. Electrodes are placed in the heart to measure electrical activity along the heart's conduction system and within heart muscle cells themselves.
Normal electrical activity is signaled from the heart's natural pacemaker known as the sinoatrial (SA) node. It then travels through the atria (the two chambers on the top of the heart), the atrioventricular (AV) node (connecting the atria to the ventricles), and the ventricles (the lower chambers of the heart).
Abnormal electrical activity can occur anywhere along this conduction system, including in the muscle cells of the atria or ventricles. The electrodes inserted during EPS will map the type of arrhythmia you have and where the problem arises in your heart. This information will allow your cardiologist to determine the severity of the problem (including whether you are at risk for sudden cardiac death) as well as appropriate treatment.
How to prepare for test
Test preparations are similar to those for a cardiac catheterization. Food and fluid will be restricted for 6 - 8 hours before the test. The procedure will take place in a hospital, and you will wear hospital clothing. You must sign a consent form for the procedure.
Your health care provider will give you instructions regarding any changes to your normal medications. Do not stop taking or change any medications without consulting your health care provider.
A mild sedative is usually given 30 minutes before the procedure. You may not be able to drive home yourself if you are discharged the same day.
How test will feel
During the test, you may be awake and able to follow instructions or sedated.
A simple EPS generally lasts from 30 minutes to an hour. It may take longer if other procedures are involved.
Why test is performed
Before performing EPS, your cardiologist will try to identify a suspected arrhythmia using other, less invasive tests such as ambulatory cardiac monitoring. If the abnormal rhythm is not detected by these other methods, and your symptoms suggest you have an arrhythmia, EPS may be recommended. Additional reasons for EPS may include the need:
• To find the location of a known arrhythmia and determine the best therapy
• To assess the severity of the arrhythmia and determine if you are at risk for future cardiac events, especially sudden cardiac death
• To evaluate the effectiveness of medication in controlling an arrhythmia
• To determine if the focus (the place from where the arrhythmia is coming) should be ablated. If ablation is appropriate, it will be formed immediately.
• To evaluate the need for a permanent pacemaker or an implantable cardioverter-defibrillator (ICD)
What abnormal results mean
The exact location and type of the arrhythmia must be determined so that specific therapy can be applied appropriately. The arrhythmia may originate from any area of the heart's electrical conduction system. For example:
• Sick sinus syndrome occurs when the SA node of the heart malfunctions
• Wolff-Parkinson-White syndrome happens when there is an extra electrical pathway, causing the signal to avoid the normal path through the AV node
• Ventricular fibrillation and ventricular tachycardia can occur when muscle cells in the ventricles inappropriately take over the electrical activity of the heart
Risks
The procedure is generally safe. Possible risks include but are not limited to the following:
• Arrhythmias
• Cardiac arrest
• Trauma to the vein
• Low blood pressure
• Infection
• Cardiac tamponade
• Embolism caused by blood clots developing at the tip of the catheter
• Bleeding
Acknowledgements
Heart Rhythm Specialists of South Florida gives special thanks to the National Library of Medicine and National Heart Lung and Blood Institute whose Web sites aided in the research of the patient educational material provided above.